REFRACTIVE SURGERY - LASIK (Laser Assisted In-Situ Keratomileusis)
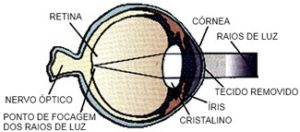 In order to undergo this technique, you must get detailed information about your refractive defect by making a personal appointment and speaking to your doctor. If your refractive defect is in the LASIK correction range, some tests will be performed. If not, the doctor may recommend another refractive procedure in order to solve your problem.
In order to undergo this technique, you must get detailed information about your refractive defect by making a personal appointment and speaking to your doctor. If your refractive defect is in the LASIK correction range, some tests will be performed. If not, the doctor may recommend another refractive procedure in order to solve your problem.Before surgery:
The surgeon will evaluate if the patient meets all the conditions to perform the surgery, taking into account several aspects that can condition the results of this surgery, such as very dilated pupils, the eye being dry or previous ocular lesions.Procedure:
The patient lies down on a reclining chair in an outpatient surgery room. The eye to be operated on is anesthetized with drops, and then a small surgical instrument (blepharostat) is placed to keep the eyelids open during surgery. A suction ring is then placed over the cornea to secure it and prevent eye movement. At this point, the patient may feel pressure from the blepharostat and their vision may become blurred. Next, the microkeratome—an automated microsurgical instrument—is attached to the suction ring. As the microkeratome blade glides over the cornea, the patient will hear a metallic sound and have poor vision. When the microkeratome stops working, a flap of tissue will have been created, which is folded back and held in place at one end. (Fig. 1) The laser is then activated at the thickness of the cornea. At this point, the patient must stare at a red light, while their vision is blurred and they hear a sound corresponding to the laser performing the ablation. (Fig. 2) Finally, the surgeon puts the flap that was folded back into place and it attaches itself without the need for stitches (Fig. 3).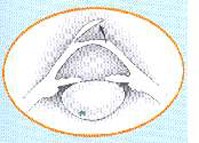
Fig.1
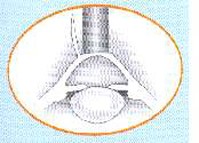
Fig.2
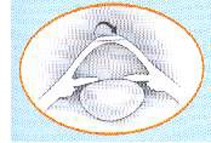
Fig.3
After surgery:
The patient will walk around with a bandaged eye for one day and will be able to resume their activity the next day. Vision will recover in the days or weeks following surgery and in some cases it may take several months to achieve the clarity of vision the patient had when wearing glasses or contact lenses.Like any other surgery, LASIK has risks and may have complications that, although very rare, should be carefully considered.
In some cases under- or over-corrections can occur. Fortunately, these can be corrected with spectacles, contact lenses or further surgery. There is still a small chance that the vision after surgery will not be as good as when wearing glasses or contact lenses.
Some people experience temporary discomfort, blurred vision, tearing, dry eye, dazzling, halos around lights, light sensitivity and fluctuating vision. These symptoms usually disappear within a month. In some cases they persist longer and may not disappear completely.
CONTACTS
COIMBRA
Rua Câmara Pestana, n.º 35-37
3030-163 Coimbra, Portugal
Tel.: +351 239 484 348
(Call to national landline)
Mobile: +351 966 320 022
(Call to national landline)
Fax: +351 239 481 487
(Call to national landline)
E-mail: emc@oftalmologia.co.pt
AVEIRO
Rufino Silva – Ophthalmology Clinic
Av. Lourenço Peixinho, No. 177-179, 2nd floor
3800 – 167 – Aveiro
Tel.: +351 234 382 847
(Call to national mobile network)
Mobile: +351 918 644 767
(Call to national mobile network)
Email: aveiro@oftalmologia.co.pt
FORM
COIMBRA
Espaço Médico de Coimbra
Rua Câmara Pestana, n.º 35-37
3030-163 Coimbra, Portugal
Phone: +351 239 484 348 /Telm: +351 966 320 022
Fax: +351 239 481 487
E-mail: emc@oftalmologia.co.pt
AVEIRO
Rufino Silva - Clínica Oftalmológica
Av. Lourenço Peixinho, Nº 177-179, 2º andar
3800 - 167 - Aveiro
Phone: +351 234 382 847
Mobile: +351 918 644 767
E-mail: aveiro@oftalmologia.co.pt
COIMBRA
Espaço Médico de Coimbra
Rua Câmara Pestana, n.º 35-37
3030-163 Coimbra, Portugal
Phone: +351 239 484 348 /Telm: +351 966 320 022
Fax: +351 239 481 487
E-mail: emc@oftalmologia.co.pt
AVEIRO
Rufino Silva - Clínica Oftalmológica
Av. Lourenço Peixinho, Nº 177-179, 2º andar
3800 - 167 - Aveiro
Phone: +351 234 382 847
Mobile: +351 918 644 767
E-mail: aveiro@oftalmologia.co.pt
















